Environmental Allergies | Vibepedia
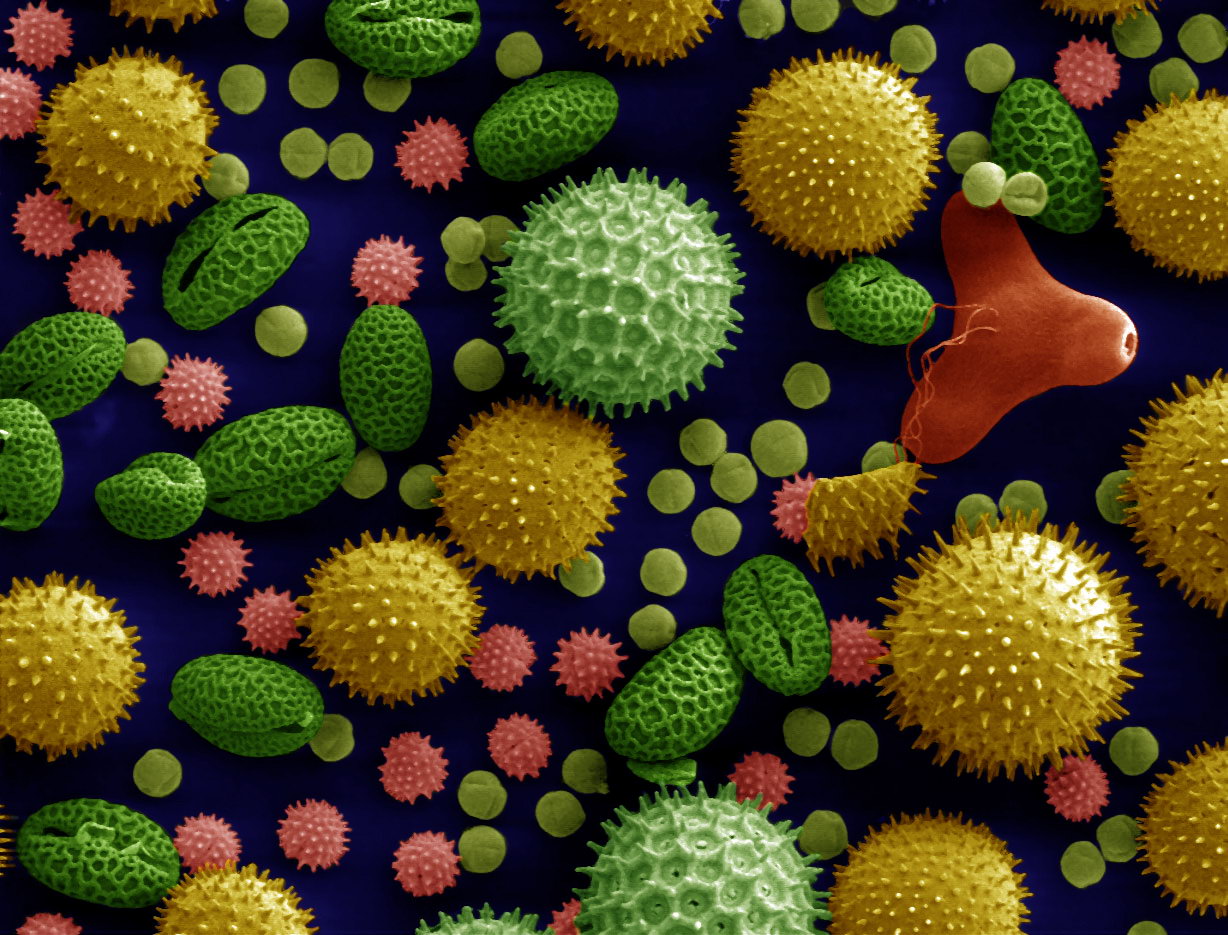
Environmental allergies, commonly known as hay fever or allergic rhinitis, represent a widespread immune system overreaction to otherwise harmless airborne…
Contents
Overview
Environmental allergies, commonly known as hay fever or allergic rhinitis, represent a widespread immune system overreaction to otherwise harmless airborne substances. These reactions, classified as Type I hypersensitivity, manifest as inflammation in the nasal passages and eyes, leading to symptoms like sneezing, itching, watery eyes, and a runny or blocked nose. Triggers range from ubiquitous pollen and dust mites to pet dander and mold spores, often exhibiting seasonal patterns tied to plant life cycles. While genetics plays a significant role in predisposition, environmental factors and exposure levels are increasingly understood to influence prevalence and severity. Millions worldwide grapple with these conditions, impacting sleep, productivity, and overall quality of life, often co-occurring with other atopic conditions like asthma and eczema.
🎵 Origins & History
The concept of the body reacting adversely to environmental elements isn't new, but the scientific understanding of allergies, particularly environmental ones, gained traction in the late 19th and early 20th centuries. The term 'hay fever' was coined for the seasonal symptoms linked to grass pollen. The identification of IgE antibodies provided the molecular mechanism, explaining how the immune system targets specific environmental allergens like ragweed pollen or house dust mites. This era also saw the rise of organizations like the American Academy of Allergy, Asthma & Immunology (AAAAI), dedicated to advancing research and clinical practice in this burgeoning field.
⚙️ How It Works
Environmental allergies function through a complex immune response initiated by mast cells and basophils. Upon initial exposure to an allergen, such as birch pollen, the immune system produces allergen-specific IgE antibodies. These IgE molecules then bind to the surface of mast cells and basophils. During subsequent exposures, the allergen binds to these IgE antibodies, triggering the release of potent inflammatory mediators like histamine, leukotrienes, and prostaglandins. These chemicals cause the characteristic symptoms: vasodilation leading to redness and swelling, increased mucus production causing a runny nose, and nerve stimulation resulting in itching and sneezing. The process is a classic example of a Type I hypersensitivity reaction, where the immune system mistakenly identifies a benign environmental substance as a threat.
📊 Key Facts & Numbers
Globally, environmental allergies affect a significant portion of the population. Pollen, a primary culprit, can contain millions of grains per square meter of air during peak seasons, with common types like oak, grass, and ragweed pollen being major offenders. Mold spores, often found in damp environments, can number in the thousands per cubic meter, exacerbating symptoms for susceptible individuals.
👥 Key People & Organizations
Pioneering figures in allergy research include Frederic Spencer Lowell, who described the clinical features of hay fever in the 19th century, and Allan P. Sullivan, who further elucidated the role of pollen. Key organizations driving research and patient advocacy include the World Allergy Organization (WAO), which promotes global awareness and research initiatives, and national bodies like the Allergy and Clinical Immunology Society of the Philippines. Pharmaceutical giants like GlaxoSmithKline and Sanofi invest heavily in developing new antihistamines and immunotherapy treatments, while academic institutions such as Johns Hopkins University and Karolinska Institute continue to push the boundaries of immunological understanding.
🌍 Cultural Impact & Influence
Environmental allergies have profoundly shaped modern lifestyles and public health discourse. The ubiquity of symptoms has normalized sneezing fits and itchy eyes in public spaces, while the economic burden has spurred significant investment in pharmaceutical research and development. The cultural narrative often portrays allergy sufferers as somewhat pitiable but relatable figures, a trope seen in countless films and television shows. Furthermore, the growing awareness of environmental allergies has contributed to a broader public understanding of the immune system and the concept of autoimmune or hypersensitive responses, influencing discussions around hygiene and exposure in early childhood development, often referred to as the hygiene hypothesis.
⚡ Current State & Latest Developments
The current landscape of environmental allergies is marked by increasing prevalence, particularly in urbanized areas, and a growing understanding of the interplay between genetics and environmental exposures. Advances in allergen immunotherapy are offering more targeted and effective long-term treatment options, including sublingual tablets for allergens like grass and ragweed. Digital health platforms are emerging, offering real-time pollen counts and personalized allergy forecasts through apps like Pollen.com and The Weather Channel app. Research is also intensifying into the microbiome's role in immune system development and its potential impact on allergy onset and severity, with studies from institutions like the University of California, San Diego exploring these connections.
🤔 Controversies & Debates
A significant debate revolves around the 'hygiene hypothesis' and its implications for childhood development. While initially positing that reduced exposure to microbes in early life leads to increased allergies, newer iterations suggest a more nuanced view involving the type of microbial exposure. Another controversy lies in the marketing and perceived necessity of over-the-counter allergy medications, with some critics arguing for greater emphasis on lifestyle changes and allergen avoidance. Furthermore, the long-term effects and accessibility of advanced treatments like biologic drugs for severe allergic conditions remain a subject of ongoing discussion and research, particularly concerning cost and patient selection.
🔮 Future Outlook & Predictions
The future of managing environmental allergies points towards highly personalized medicine and advanced preventative strategies. Gene editing technologies and sophisticated biomarker discovery may allow for earlier identification of individuals at high risk and the development of targeted interventions before symptoms manifest. The development of allergen-specific immunotherapy delivered via novel methods, such as microneedle patches, could improve patient compliance and efficacy. Predictive modeling using AI, integrating data from wearable sensors, environmental monitoring, and genetic profiles, could offer hyper-local, real-time allergy forecasts and personalized avoidance advice, potentially mitigating the impact of allergens like dust mites and pet dander on a global scale.
💡 Practical Applications
Environmental allergies have direct practical applications in public health and personal well-being. Understanding allergen triggers allows for effective allergen avoidance strategies, such as keeping windows closed during high pollen seasons, using HEPA air purifiers to filter indoor allergens, and regular cleaning to reduce dust mite populations. Pharmacological interventions, including loratadine (Claritin) and fexofenadine (Allegra), provide symptomatic relief. For persistent cases, allergen immunotherapy (allergy shots or sublingual tablets) offers a way to desensitize the immune system to specific allergens like cat dander or cockroach allergens, reducing reliance on medication. Diagnostic tools like skin prick tests and blood tests (e.g., ImmunoCAP) are crucial for accurate diagnosis.
Key Facts
- Category
- science
- Type
- topic