Premature Birth | Vibepedia
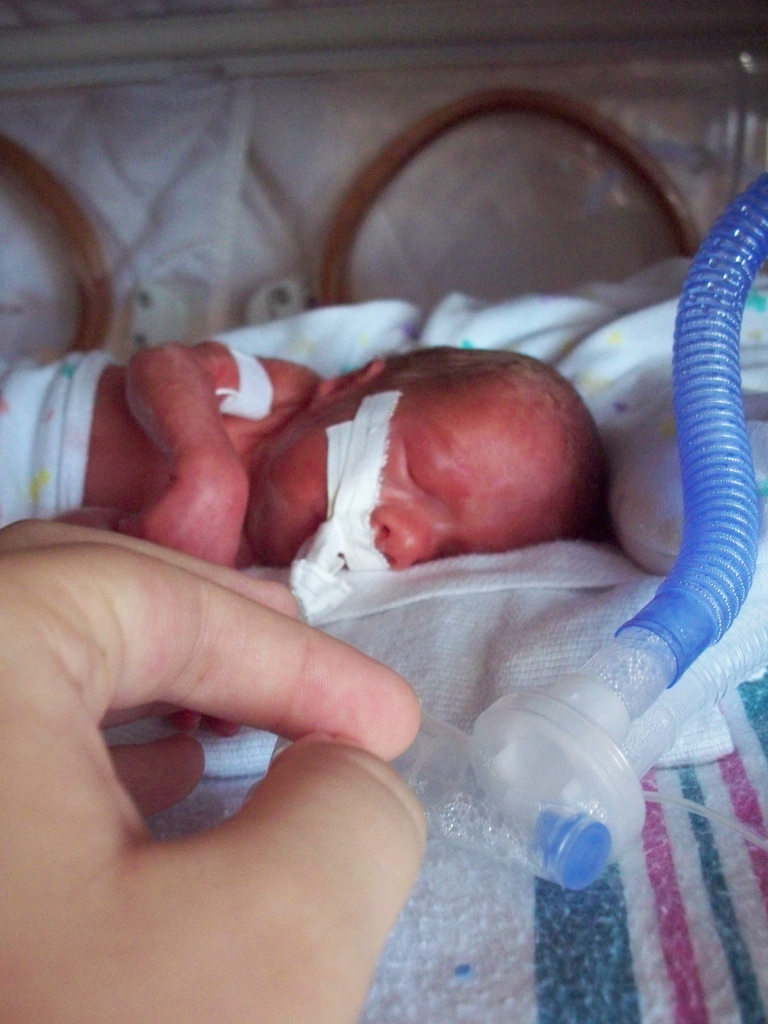
Premature birth, defined as delivery before 37 completed weeks of gestation, represents a critical challenge in modern obstetrics and neonatology. These…
Contents
Overview
Premature birth, defined as delivery before 37 completed weeks of gestation, represents a critical challenge in modern obstetrics and neonatology. These infants, often termed 'preemies' or 'premmies,' face significantly elevated risks for a spectrum of health issues, ranging from developmental delays and sensory impairments to severe neurological conditions like cerebral palsy. The earlier the birth, the more pronounced these risks become, with extreme prematurity (under 28 weeks) carrying the gravest prognoses. While spontaneous preterm labor often lacks a clear etiology, known risk factors include maternal conditions such as diabetes and hypertension, multiple gestations, and certain infections. Globally, an estimated 15 million babies are born prematurely each year, making it a leading cause of neonatal mortality and a significant contributor to long-term disability, impacting families and healthcare systems worldwide. The ongoing scientific and medical efforts focus on prevention, improved neonatal care, and understanding the intricate biological pathways that trigger early labor.
🎵 Origins & History
The concept of birth occurring significantly before the expected term has been a recognized medical concern for centuries, though understanding and intervention capabilities have evolved dramatically. Ancient Greek physicians like Hippocrates noted variations in gestation length, and early medical texts described infants born "too soon." However, systematic study and classification are more recent. The formal definition of prematurity, typically set at less than 37 weeks of gestation, gained traction in the 20th century with advancements in neonatal care and a growing understanding of fetal development. The establishment of specialized neonatal intensive care units (NICUs) marked a turning point, offering previously impossible levels of support for extremely premature infants. Early efforts focused on basic survival, while later research, particularly from institutions like the National Institutes of Health (NIH), began to unravel the complex biological triggers of preterm labor.
⚙️ How It Works
Premature birth occurs when the physiological processes that signal the end of pregnancy are initiated before the fetus has reached full term, typically defined as 37 weeks of gestation. This can manifest as spontaneous preterm labor, characterized by regular uterine contractions that cause cervical change, or as medically indicated preterm birth, often necessitated by maternal or fetal complications such as preeclampsia or placental abruption. The exact cascade of events leading to spontaneous preterm labor is multifaceted and not fully understood, but it often involves premature activation of the maternal or fetal hypothalamic-pituitary-adrenal (HPA) axis, uterine inflammation, or cervical insufficiency. The immature organ systems of a premature infant—including the lungs, brain, and gastrointestinal tract—are ill-equipped to handle extrauterine life, necessitating intensive medical support in a NICU setting to manage breathing, feeding, temperature regulation, and infection prevention.
📊 Key Facts & Numbers
Globally, an estimated 15 million babies are born prematurely each year, accounting for over 10% of all births worldwide. This translates to approximately one in every eight births being preterm. The burden is disproportionately higher in low- and middle-income countries, where access to prenatal care and neonatal support is limited. In the United States, the preterm birth rate was around 10.5% in 2022, a figure that has seen a slight decline but remains a significant public health concern. Babies born between 28 and 32 weeks' gestation are classified as very preterm, while those born before 28 weeks are considered extremely preterm. The survival rates for these infants vary dramatically; for example, survival rates for babies born at 24 weeks' gestation can be as low as 50-60% in high-resource settings, and significantly lower elsewhere. The economic cost is also substantial, with NICU stays for premature infants often costing tens of thousands of dollars per day.
👥 Key People & Organizations
Key figures in the fight against premature birth include neonatologists, obstetricians, and researchers dedicated to improving outcomes. Dr. Ferdinand Klaus, often called the "father of neonatology," was instrumental in developing NICU care standards. Organizations like the March of Dimes have been pivotal in funding research, raising public awareness, and advocating for policies to reduce preterm birth rates. The World Health Organization (WHO) plays a crucial role in global data collection and setting international guidelines for maternal and newborn care. Researchers at institutions such as the University of Pennsylvania and the Stanford University School of Medicine are actively investigating the genetic and environmental factors contributing to preterm birth. The American Academy of Pediatrics provides clinical guidelines for the care of premature infants.
🌍 Cultural Impact & Influence
Premature birth has a profound cultural resonance, often evoking strong emotional responses related to vulnerability, hope, and the fragility of life. The "preemie" experience has been depicted in numerous films and television shows, highlighting the intense emotional journeys of parents and the medical challenges faced by these tiny infants. Celebrities like Kim Kardashian have publicly shared their experiences with premature births, bringing greater awareness to the issue. The "Prematurity Awareness Month" in November aims to educate the public and advocate for support systems for families. Culturally, the image of the "miracle baby"—a premature infant who overcomes immense odds—is a powerful narrative that underscores the resilience of both the child and the medical teams involved. However, the long-term challenges faced by survivors, such as chronic health conditions and developmental disabilities, also represent a significant societal impact that extends far beyond the initial birth.
⚡ Current State & Latest Developments
Current efforts in managing premature birth focus on both prevention and improved neonatal care. Advanced prenatal care strategies, including progesterone supplementation for high-risk pregnancies and the use of fetal fibronectin tests to predict imminent labor, are being refined. In neonatal intensive care, breakthroughs in mechanical ventilation techniques, surfactant therapy to mature lungs, and nutritional support have significantly improved survival rates for very preterm infants. The development of neonatal robotic surgery is also expanding treatment options for complex congenital conditions in premature babies. Organizations like the National Preterm Birth Initiative are collaborating across states to implement evidence-based interventions aimed at reducing preterm birth rates. Ongoing research continues to explore the role of the maternal gut microbiome and inflammation in triggering preterm labor, with studies from institutions like the University of California, San Francisco showing promising links.
🤔 Controversies & Debates
A significant debate surrounds the optimal timing and intensity of interventions for extremely premature infants. While survival rates have improved, questions persist about the long-term quality of life for survivors, leading to ethical discussions about aggressive medicalization versus palliative care. The role of in vitro fertilization (IVF) and other assisted reproductive technologies in the rise of multiple gestations, a known risk factor for preterm birth, is another area of ongoing discussion. Furthermore, disparities in preterm birth rates across racial and socioeconomic groups, particularly the higher rates among Black women in the United States, are a subject of intense debate, with researchers exploring the complex interplay of systemic racism, stress, and access to care as contributing factors. The definition of "viability"—the point at which a fetus can survive outside the womb—also remains a point of contention, influencing medical decisions and legal frameworks.
🔮 Future Outlook & Predictions
The future of premature birth management is likely to involve a combination of enhanced preventative strategies and more personalized, technologically advanced neonatal care. Gene editing technologies and advanced stem cell therapies may offer novel approaches to address organ immaturity and repair damage in premature infants. Predictive analytics, leveraging big data from electronic health records and wearable sensors, could enable earlier identification of at-risk pregnancies. Researchers are also exploring novel pharmacological intervent
Key Facts
- Category
- science
- Type
- topic